Treatment for Morton's Neuroma
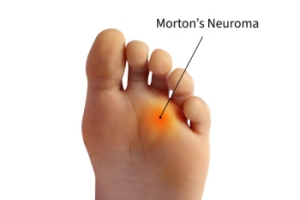
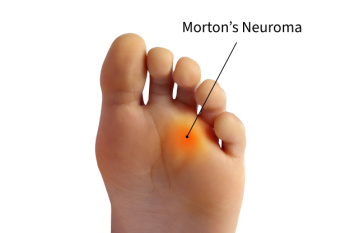 Morton’s neuroma is a painful condition that affects the ball of the foot, typically between the third and fourth toes. It involves the thickening of tissue around one of the nerves leading to the toes, often caused by irritation or compression. Symptoms include a sharp, burning pain in the ball of the foot, tingling or numbness in the toes, and the sensation of having a pebble in your shoe. A podiatrist diagnoses Morton's neuroma through a physical examination, assessing the affected area for tenderness and swelling. Imaging tests such as X-rays, ultrasound, or MRI scans may be used to rule out other conditions. The duration of symptoms can vary, with some people experiencing intermittent pain while others may have chronic discomfort. Prevention includes wearing well-fitting shoes with a wide toe box and avoiding high heels. Treatment options range from conservative approaches like rest and orthotics to corticosteroid injections and, in severe cases, surgery. For persistent pain and personalized treatment, it is suggested that you schedule an appointment with a podiatrist.
Morton’s neuroma is a painful condition that affects the ball of the foot, typically between the third and fourth toes. It involves the thickening of tissue around one of the nerves leading to the toes, often caused by irritation or compression. Symptoms include a sharp, burning pain in the ball of the foot, tingling or numbness in the toes, and the sensation of having a pebble in your shoe. A podiatrist diagnoses Morton's neuroma through a physical examination, assessing the affected area for tenderness and swelling. Imaging tests such as X-rays, ultrasound, or MRI scans may be used to rule out other conditions. The duration of symptoms can vary, with some people experiencing intermittent pain while others may have chronic discomfort. Prevention includes wearing well-fitting shoes with a wide toe box and avoiding high heels. Treatment options range from conservative approaches like rest and orthotics to corticosteroid injections and, in severe cases, surgery. For persistent pain and personalized treatment, it is suggested that you schedule an appointment with a podiatrist.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact one of our doctors of Coral Desert Foot & Ankle. Our doctors will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact one of our offices located in St. George and Kanab, UT, and Mesquite, NV . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What is Morton's Neuroma?
Morton’s neuroma, (also referred to as Morton’s metatarsalgia, Morton’s neuralgia, plantar neuroma or intermetatarsal neuroma) is a condition that is caused when the tissue around one of the nerves between your toes begins to thicken. This thickening can result in pain in the ball of the foot. Fortunately, the condition itself is not cancerous.
Morton’s neuroma affects women more often than men with a ratio of 4:1. It tends to target women between the age of 50 and 60, but it can occur in people of all ages. There are some risk factors that may put you at a slightly higher risk of developing the condition. People who often wear narrow or high-heeled shoes are often found to be linked to Morton’s neuroma. Additionally, activities such as running or jogging can put an enormous amount of pressure on the ligament and cause the nerve to thicken.
There usually aren’t any outward symptoms of this condition. A person who has Morton’s neuroma may feel as if they are standing on a pebble in their shoe. They may also feel a tingling or numbness in the toes as well as a burning pain in the ball of their foot that may radiate to their toes.
In order to properly diagnose you, the doctor will press on your foot to feel for a mass or tender spot. He may also do a series of tests such as x-rays, an ultrasound, or an MRI. X-rays are usually done to rule out any other causes for your foot pain such as a stress fracture. Ultrasounds are used to reveal soft tissue abnormalities that may exist, such as neuromas. Your podiatrist may want to use an MRI in order to visualize your soft tissues.
There are three main options for treatment of Morton’s neuroma: Injections, decompression surgery, and removal of the nerve. Injections of steroids into the painful area have been proven to help those with Morton’s neuroma. Decompression surgery has been shown to relieve pressure on the affected nerve by cutting nearby structures such as the ligaments in the foot. Another treatment option would be to surgically remove the growth to provide pain relief.
If you suspect that you have Morton’s neuroma you should make an appointment with your podiatrist right away. You shouldn’t ignore any foot pain that lasts longer than a few days, especially if the pain does not improve.
Essential Stretches to Prevent Running and Jogging Injuries

To maintain peak performance and prevent injuries while running or jogging, incorporating a comprehensive stretching routine is vital. The feet and ankles may become stronger when stretches are implemented before and after the workout, which may help to prevent running injuries. Dynamic stretches, performed before the workout, help prepare the muscles for activity by increasing blood flow and range of motion. Leg swings, lunges with a twist, and hip circles are dynamic stretches that target key muscle groups involved in running and jogging. Post-workout, static stretches aid in muscle recovery and flexibility by holding positions that target specific muscle groups for 15 to 30 seconds each. Essential static stretches include calf stretches, hamstring stretches, quadriceps stretches, and hip flexor stretches. Additionally, incorporating yoga poses such as downward-facing dog, pigeon pose, and runner’s lunge can further enhance flexibility and prevent tightness and imbalances. If you have endured a foot or ankle injury while running, it is suggested that you contact a podiatrist for relief strategies.
Exercising your feet regularly with the proper foot wear is a great way to prevent injuries. If you have any concerns about your feet, contact one of our doctors of Coral Desert Foot & Ankle. Our doctors will treat your foot and ankle needs.
How to Prevent Running Injuries
Many common running injuries are caused by overuse and overtraining. When the back of the kneecap starts wearing out and starts causing pain in your knee, this is commonly referred to as runner’s knee. Runner’s knee is a decrease in strength in your quadriceps and can occur if you’re not wearing properly fitted or supporting shoes. To prevent runner’s knee, focusing on hip strengthening is a good idea, as well as strengthening your quads to keep the kneecaps aligned.
What Are Some Causes of Running Injuries?
- One cause of a common running injury is called iliotibial band syndrome.
- Plantar fasciitis is also another common injury.
- Stress fractures can occur from overtraining, lack of calcium, or even your running style.
Best Ways to Prevent Running Injuries
- Wear footwear that fits properly and suits your running needs.
- Running shoes are the only protective gear that runners have to safeguard them from injury.
- Make a training schedule. Adding strengthening exercises as well as regular stretching can help keep you strong and limber and can lessen the possibility of injuries.
- Stretching keeps muscles limber; this will help you gain better flexibility.
If you have any questions please feel free to contact one of our offices located in St. George and Kanab, UT, and Mesquite, NV . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Prevent Running Injuries
Overtraining and overusing the feet are the main causes of common running injuries. A number of these common injuries are caused by overrunning. Runner’s knee is a condition that is characterized by the back of the kneecap beginning to wear away and cause pain in the knee. This frequently occurs due to either a decrease in strength in the quadriceps muscles or ill-fitting shoes that are lacking in proper support for the inside of the forefoot. Strengthening exercises focusing on the quad muscle and sports orthotics are the usual treatments for those suffering from runner’s knee. Prevention of the condition lies in a focus on hip strengthening and quad-strengthening to keep the kneecap aligned. To help learn the best exercise to heal runner’s knee, one can also undergo physical therapy.
One common injury, called iliotibial band syndrome, is often caused by overtraining. This condition occurs when the iliotibial band gets irritated, creating pain and discomfort in the outside knee area. Plantar fasciitis, another common running injury, also occurs as a result of inflammation and irritation. Plantar fasciitis is an inflammation and irritation of the bone in the foot. A large amount of pain is often experienced due to plantar fasciitis. The condition can be caused by a high arch, improper footwear, tight muscles, or flat feet. It can best be avoided by stretching and wearing appropriate footwear that supports the foot.
Another common injury for runners is stress fractures. These injuries occur due to running style, overtraining, or a lack of calcium. Stress fractures most often occur in several locations in runners, including the inner bone of the leg, the thighbone, the bone at the base of the spine and the bones of the toes. Stress fractures are best prevented by wearing proper footwear and by running on flat and hard surfaces; this will absorb some of the shock created during running.
Aside from overtraining, other causes of common running injuries include ill-fitting footwear, a lack of flexibility and strength, and irregular biomechanics. The best way to avoid running injuries is to prevent them from even occurring. Both iliotibial band syndrome and stress fractures are preventable. The first step that should be taken to prevent running injuries is to only wear footwear that fits properly and that is appropriate for whatever activity you are doing. Running shoes are the only protective gear available to runners that can safeguard them from sustaining injuries. Choosing the right pair of shoes is therefore extremely important. While running shoes are an important factor, it is also important to consider other facets of your running routine such as training schedules, flexibility, and strengthening. These elements should be considered and altered according to your running needs to best maximize your run and minimize the possibility of injury. Careful stretching before and after a run should also be considered to help prevent running injuries. Stretching muscles enables greater flexibility and a lesser chance of sustaining injury.
Keep Your Feet Healthy So You Can Stay Active
Gout Management Techniques
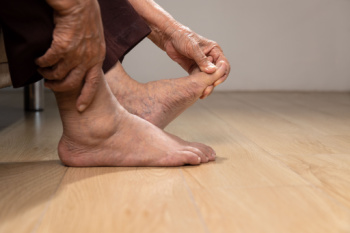 Gout is a form of arthritis characterized by sudden, severe attacks of pain, swelling, and redness in the joints. These symptoms often occur in the big toe. Treatment focuses on relieving pain during attacks and preventing future episodes. A podiatrist, or foot doctor, may recommend medications like nonsteroidal anti-inflammatory drugs, colchicine, or corticosteroids to reduce inflammation and pain during acute flare-ups. To manage gout long-term, changes in diet and lifestyle, such as reducing intake of high-purine foods, like red meat and seafood, increasing hydration, and maintaining a healthy weight, are important. A podiatrist can also suggest footwear designed to alleviate pressure on the affected joints, which may involve the use of orthotic devices for extra cushioning and support. Longer-term management techniques may involve the prescription of urate-lowering medications to decrease levels of uric acid in the blood. This helps to prevent the formation of urate crystals that cause gout symptoms. Regular follow-ups with a podiatrist are important to monitor gout symptoms and adjust treatment plans as needed. If you have gout, it is suggested that you consult with a podiatrist for targeted treatment.
Gout is a form of arthritis characterized by sudden, severe attacks of pain, swelling, and redness in the joints. These symptoms often occur in the big toe. Treatment focuses on relieving pain during attacks and preventing future episodes. A podiatrist, or foot doctor, may recommend medications like nonsteroidal anti-inflammatory drugs, colchicine, or corticosteroids to reduce inflammation and pain during acute flare-ups. To manage gout long-term, changes in diet and lifestyle, such as reducing intake of high-purine foods, like red meat and seafood, increasing hydration, and maintaining a healthy weight, are important. A podiatrist can also suggest footwear designed to alleviate pressure on the affected joints, which may involve the use of orthotic devices for extra cushioning and support. Longer-term management techniques may involve the prescription of urate-lowering medications to decrease levels of uric acid in the blood. This helps to prevent the formation of urate crystals that cause gout symptoms. Regular follow-ups with a podiatrist are important to monitor gout symptoms and adjust treatment plans as needed. If you have gout, it is suggested that you consult with a podiatrist for targeted treatment.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact one of our doctors from Coral Desert Foot & Ankle. Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact one of our offices located in St. George and Kanab, UT, and Mesquite, NV . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Everything You Need to Know About Gout
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
Symptoms of Toenail Fungus
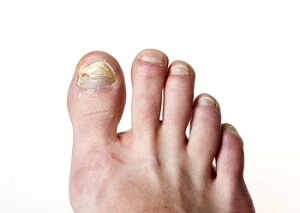
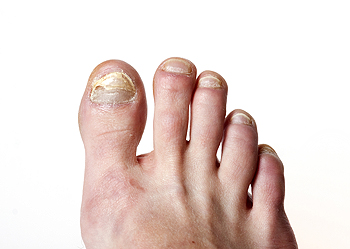 Toenail fungus, also known as onychomycosis, has several distinct symptoms that can affect the appearance and health of your toenails. The infection usually starts with a white or yellow spot under the tip of the toenail. As it progresses, the fungus can cause the nail to discolor, thicken, and develop crumbling edges. This may make the nail difficult to trim. The affected nails may also become brittle, ragged, and take on a dull, lackluster appearance. In some cases, the nail can separate from the nail bed. This may be a painful experience and can lead to further complications. Advanced cases of toenail fungus can result in a foul odor. A podiatrist, or foot doctor, can recommend effective treatments. These often include antifungal medications, topical treatments, and, in severe instances, professional removal of the nail. If you suspect toenail fungus, it is suggested that you schedule an appointment with a podiatrist to discuss treatment options.
Toenail fungus, also known as onychomycosis, has several distinct symptoms that can affect the appearance and health of your toenails. The infection usually starts with a white or yellow spot under the tip of the toenail. As it progresses, the fungus can cause the nail to discolor, thicken, and develop crumbling edges. This may make the nail difficult to trim. The affected nails may also become brittle, ragged, and take on a dull, lackluster appearance. In some cases, the nail can separate from the nail bed. This may be a painful experience and can lead to further complications. Advanced cases of toenail fungus can result in a foul odor. A podiatrist, or foot doctor, can recommend effective treatments. These often include antifungal medications, topical treatments, and, in severe instances, professional removal of the nail. If you suspect toenail fungus, it is suggested that you schedule an appointment with a podiatrist to discuss treatment options.
For more information about treatment, contact one of our doctors of Coral Desert Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact one of our offices located in St. George and Kanab, UT, and Mesquite, NV . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
How to Treat Your Toenail Fungus
While not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
Broken Toe Causes and Treatment
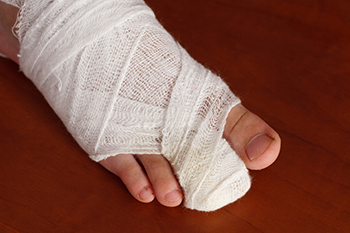
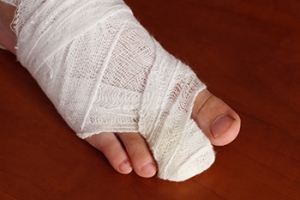
Broken toes, or toe fractures, typically occur when the toe experiences a sudden impact or pressure. This may be due to a heavy object falling on it or stubbing it against a hard surface, like furniture or steps. Symptoms of a broken toe include pain, swelling, and discoloration of the toenail because of trapped blood underneath. Fractures of the big toe potentially cause more intense pain, increased swelling, and bruising, which affects mobility. Diagnosis of a fractured toe is usually made through a physical examination by a podiatrist, often without the need for X-rays. Treatment may involve buddy taping, which is securing the injured toe to the adjacent one for support. Draining trapped blood under the toenail to help alleviate discomfort. A podiatrist also may prescribe wearing comfortable footwear or a protective boot to aid healing. In more serious cases, surgery may be required to correct the injury. For an exam, personalized guidance, and proper treatment of a broken toe, it is suggested that you schedule an appointment with a podiatrist.
A broken toe can be very painful and lead to complications if not properly fixed. If you have any concerns about your feet, contact one of our doctors from Coral Desert Foot & Ankle. Our doctors will treat your foot and ankle needs.
What to Know About a Broken Toe
Although most people try to avoid foot trauma such as banging, stubbing, or dropping heavy objects on their feet, the unfortunate fact is that it is a common occurrence. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break (fracture).
Symptoms of a Broken Toe
- Throbbing pain
- Swelling
- Bruising on the skin and toenail
- The inability to move the toe
- Toe appears crooked or disfigured
- Tingling or numbness in the toe
Generally, it is best to stay off of the injured toe with the affected foot elevated.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery. Due to its position and the pressure it endures with daily activity, future complications can occur if the big toe is not properly treated.
If you have any questions please feel free to contact one of our offices located in St. George and Kanab, UT, and Mesquite, NV . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.